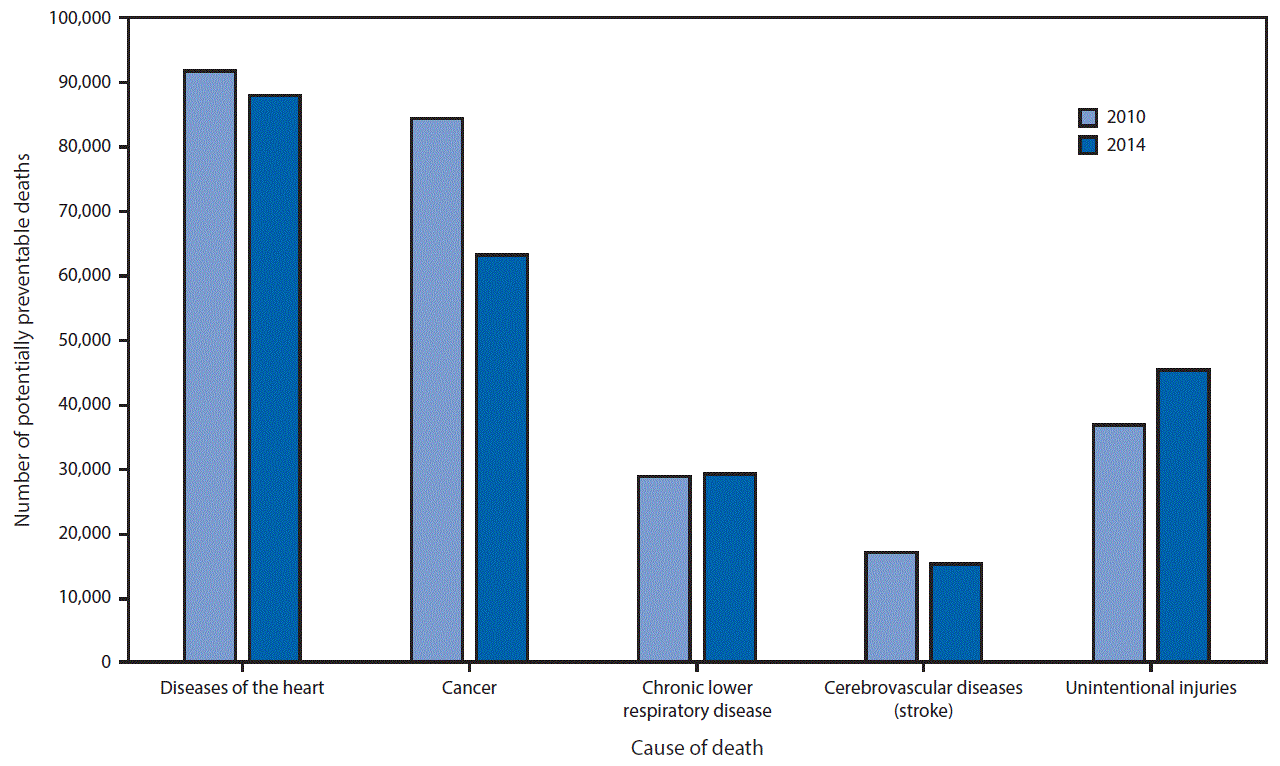
Potentially Preventable Deaths Among the Five Leading Causes of Death — United States, 2010 and 2014Weekly / November 18, 2016 / 65(45);1245–1255 Article MetricsViews equals page views plus PDF downloadsViews:Citations:Altmetric:Metric DetailsMacarena C. García, DrPH1; Brigham Bastian2; Lauren M. Rossen, PhD2; Robert Anderson, PhD2; Arialdi Miniño, MPH2; Paula W. Yoon, ScD1; Mark Faul, PhD3; Greta Massetti, PhD4; Cheryll C. Thomas, MSPH4; Yuling Hong, MD4; Michael F. Iademarco, MD1 (View author affiliations) View suggested citationSummaryWhat is already known about this topic? Deaths from heart disease, cancer, chronic lower respiratory disease, cerebrovascular diseases (stroke), and unintentional injuries account for the five leading causes of death in the United States. Death rates for these diseases vary widely across states, related to variation in the distribution of social determinants of health, access and use of health services, and public health efforts. What is added by this report? There has been a significant decrease in the number of potentially preventable deaths among three of the five leading causes of death (diseases of the heart, cancer, and stroke) during 2010–2014. However, the number of potentially preventable deaths from unintentional injuries increased significantly during the same period. This is mostly attributed to an increase in drug poisoning (overdose from prescription and illicit drugs) and falls. No significant change was observed in potentially preventable deaths from chronic lower respiratory disease (e.g., asthma, bronchitis, and emphysema). What are the implications for public health practice? Public health officials can use the decreases observed as benchmarks for improving population health, while using observed increases to direct targeted efforts to reduce the number of potentially preventable deaths. A joint effort of public health and health care organizations can support analysis and action to reduce the number of potentially preventable deaths from the five leading causes of death. Specifically, given the reported increase in potentially preventable deaths from unintentional injuries, these findings might inform the selection and implementation of evidence-based interventions to prevent deaths from injuries such as falls and drug overdoses, based on epidemiologic burden. Death rates by specific causes vary across the 50 states and the District of Columbia.* Information on differences in rates for the leading causes of death among states might help state health officials determine prevention goals, priorities, and strategies. CDC analyzed National Vital Statistics System data to provide national and state-specific estimates of potentially preventable deaths among the five leading causes of death in 2014 and compared these estimates with estimates previously published for 2010. Compared with 2010, the estimated number of potentially preventable deaths changed (supplemental material at https://stacks.cdc.gov/view/cdc/42472); cancer deaths decreased 25% (from 84,443 to 63,209), stroke deaths decreased 11% (from 16,973 to 15,175), heart disease deaths decreased 4% (from 91,757 to 87,950), chronic lower respiratory disease (CLRD) (e.g., asthma, bronchitis, and emphysema) deaths increased 1% (from 28,831 to 29,232), and deaths from unintentional injuries increased 23% (from 36,836 to 45,331). A better understanding of progress made in reducing potentially preventable deaths in the United States might inform state and regional efforts targeting the prevention of premature deaths from the five leading causes in the United States. To determine significant changes in the number of potentially preventable deaths for the five leading causes of death in the United States, CDC analyzed National Vital Statistics System mortality data from 2014 (1) using the same analytic model presented in the original report that used 2010 data as benchmarks (2). The number of potentially preventable deaths per year per state in persons aged <80 years was determined by comparing the number of expected deaths (based on the cause-specific average death rate of the three states with the lowest 2008–2010 average rate by age groups) with the number of observed deaths in 2010 and 2014. Further detail on age-adjusted rates by state and cause can be found in yearly publications on final death data (1). Population estimates for 2010 and 2014 were produced by the U.S. Census Bureau. The calculations of potentially preventable deaths were restricted to U.S. residents and deaths in persons aged <80 years. Premature death was defined as a death that occurred in a person aged <80 years, based on the average life expectancy for the total U.S. population, which was nearly 79 years in 2010 (2). Analysis was restricted to deaths with an underlying cause of death among the five leading causes, based on International Classification of Diseases, 10th Revision (ICD-10) codes.† The five leading causes of death represented 63% of all deaths in 2014, a decrease of 2.3% compared with 2010. In 2014 the next five most frequent causes accounted for approximately 12% of deaths (3). The number of potentially preventable deaths for each of the five leading causes of death by state in 2014 was calculated in four steps. The first step was to calculate and rank state disease-specific death rates by age group. Using 2008–2010 data, the three states with the lowest observed death rates for each age group and specific cause of death category were selected and their death rates averaged across the three states to calculate a lowest average age-specific death rate for each cause of death. For example, during 2008–10, among persons aged 40–49 years, the three states with the lowest rate of death from unintentional injuries were Maryland, New Jersey, and New York, and the benchmark average was 25.2 (supplemental material at https://stacks.cdc.gov/view/cdc/42342). The average of the lowest three states was chosen to minimize the effect of any extreme outlier and to represent the low end of the distribution of death rates among the states. The second step was to calculate expected deaths for each age group and state by multiplying the age-specific state populations for 2010 by the 2010 benchmark death rates (i.e., the lowest three-state average age-specific death rates for each cause). Total expected deaths for each cause and state were calculated by summing expected deaths over all age groups aged <80 years, effectively taking into account differences in mortality across age groups. These state-specific and cause-specific expected death counts represent the number of deaths expected if all states were to achieve the 2010 death rate benchmarks (2). Third, the 2010 potentially preventable deaths were calculated by subtracting expected deaths from 2010 observed deaths. Finally, the same 2010 benchmark death rates for each cause were used to calculate 2014 potentially preventable deaths by repeating the third and fourth steps with 2014 population and mortality data. Specifically, the number of expected deaths in 2014 was calculated by multiplying the 2010 benchmark death rates by the 2014 age-specific populations; these expected counts were then subtracted from 2014 observed deaths. The numbers of potentially preventable deaths for each cause were assumed to follow a Poisson distribution, and standard errors were calculated, taking into account stochastic variation, consistent with methods described previously (2), in both the expected and observed number of deaths,§ for each cause and year. Statistically significant changes from 2010–2014 were assessed using a two-sided z-test (p<0.01). Results are presented for the United States as a whole, by state, and by the 10 U.S. Department of Health and Human Services regions.¶ The five leading causes of death for persons aged <80 years in 2014 (diseases of the heart, malignancies [cancer], cerebrovascular diseases [stroke], chronic lower respiratory diseases [CLRD], and unintentional injuries [accidents]) represent 63% of deaths from all causes. The estimated number of potentially preventable deaths and the proportion preventable among the five leading causes of death in persons aged <80 years were 87,950 for diseases of the heart (30% preventable); 63,209 for cancer (15% preventable); 45,331 for unintentional injuries (43% preventable); 29,232 for CLRD (36% preventable); and 15,175 for stroke (28% preventable) (Figure). Potentially preventable deaths from cancer declined 25% from 2010 to 2014 (the increase in the expected number of deaths was greater than the increase in the observed number). This decline appears to be driven by a 12% decrease in the age-adjusted death rate from lung cancer from 2010 and 2014. Decreases in age-adjusted death rates from cancer were observed across all U.S. states, except the District of Columbia (supplemental material at https://stacks.cdc.gov/view/cdc/42343). The expected number of deaths was based on benchmark death rates from 2010; however, cancer-related death rates declined during 2010–2014. In both 2010 and 2014 the Southeast (Region 4) had the highest number of potentially preventable deaths for each of the five leading causes of death (Table 1). In 2014, the Northwest (Region 10) had the lowest number of potentially preventable deaths for each of the five leading causes of death except deaths from CLRD and unintentional injuries, where the lowest number occurred in New York and New Jersey (Region 3) (Table 2). Consistent with increases in population since 2010, particularly among older age groups, the number of observed deaths increased for each of the five leading causes of deaths in 2014, and age-adjusted death rates declined during 2010–2014 for each category except unintentional injuries. Specifically, from 2010 to 2014, age-adjusted death rates per 100,000 population for heart disease declined 6.8% from 179.1 to 167.0; for cancer, from 172.8 to 161.2 (6.7% decrease); for stroke, from 39.1 to 36.5 (6.6% decrease); and for CLRD, from 42.2 to 40.5 (4.0% decrease). For unintentional injuries, age-adjusted death rates increased 6.6%, from 38.0 to 40.5 (supplemental material at https://stacks.cdc.gov/view/cdc/42341) (1). Among subcategories of unintentional injury deaths for all ages, age-adjusted death rates for poisonings increased 25%, and falls increased by 12% (supplemental material at https://stacks.cdc.gov/view/cdc/42344). Prescription drug and illicit drug overdose was a major contributor to the increase in poisonings during 2010–2014 (4). DiscussionThe results of this analysis show that the number of observed deaths increased for each of the leading five causes of death, consistent with increases in population size in 2014, compared with 2010. Age-adjusted death rates declined overall for all causes of death combined in 2014 compared with 2010. Potentially preventable deaths declined during 2010–2014 for three of the five leading causes of death: diseases of the heart, cancer, and stroke. No change was observed for potentially preventable deaths from CLRD. Potentially preventable deaths from unintentional injuries increased from 2010 compared with 2014. States in the Southeast continued to have the highest number of potentially preventable deaths from all five causes in 2014. Although substantial progress was made in combatting infectious diseases during the early part of the 20th century, additional focus has shifted toward prevention of noncommunicable diseases, including chronic diseases, and unintentional injuries (5,6). The decrease in cancer deaths can be attributed, in part, to progress in prevention, early detection, and treatment (7). Improvement of quality of care and reduction in risk factors, including increased number of persons with hypertension under control, have contributed to the decline in death rates for heart disease and stroke.** Tobacco use is a risk factor for some of the deaths included in this report, such as heart disease, cancer, CLRD, and cerebrovascular diseases.†† Mortality from tobacco-related causes has decreased in conjunction with national decreases in tobacco use across the United States, but an estimated 40 million adults (16.8%) smoked in 2014 (8). Implementation of evidence-based tobacco control interventions, including increased tobacco product prices, implementation and enforcement of comprehensive smoke-free laws, media campaigns, and access to proven resources (e.g., quit lines) to help persons quit tobacco use§§ varies among states. In addition to tobacco use, other health behaviors contribute to premature deaths and create opportunities for prevention. For example, obesity increases the risk for CLRD, diseases of the heart, and cerebrovascular disease, in addition to some cancers.¶¶ Although the number of potentially preventable deaths declined during 2010–2014 for heart disease, cancer, and stroke, observed deaths increased overall for these causes. Based on the methodology used for this analysis, when the pace of the increase in observed deaths is slower than the growth in population, potentially preventable deaths will decrease. Observed deaths increased 6% for heart disease, 4% for cancer, 4% for stroke, and 8% for CLRD. These increases were smaller than would be expected to result from population growth, particularly growth in population size among older age groups during this period. In contrast, both observed and potentially preventable deaths from unintentional injuries increased during 2010–2014. Examples of state actions to reduce drug overdose include developing or enhancing prescription drug monitoring programs, adopting clinical prescribing guidelines, and increasing access to medication-assisted treatment for opioid use disorder and naloxone to reverse opioid-related poisoning (9). As the U.S. population aged, falls among older adults increased. Tools such as STEADI, designed to assist clinicians in assessing fall risk, educating patients, and selecting interventions, are available from CDC.*** The findings in this report are subject to at least five limitations. First, the same method used in a previous report was applied to set a benchmark for potentially preventable deaths (2). These benchmarks are based on data from the states with the lowest death rates for each condition during 2008–2010 alone. The benchmarks might need to be reevaluated over time, especially given shifts in cause-specific death rates observed using provisional mortality data from 2015–2016.††† For example, death rates from unintentional injury were increasing before 2008–2010, resulting in benchmarks that might not be comparable to historical lows or international points of reference. Second, alternative ways of defining and measuring potentially preventable or premature avoidable mortality have been used in other studies and no gold standard exists (10). Third, a lowest average rate was calculated based on individual states. The sum of the individual potentially preventable deaths by state is qualitatively different from estimating the number of potentially preventable deaths for the United States as a whole. Fourth, changes in the number of potentially preventable deaths by cause are not necessarily independent. For example, whereas some cancer deaths might be prevented entirely, some might be shifted into another cause grouping, such as heart disease. Finally, defining potentially preventable deaths across the five leading causes does not take into consideration the fact that these are complex and diverse causes of death. Not all deaths are equivalently preventable across the leading causes or within each leading cause. For example, certain types of cancer might be considered more or less preventable than other types, and some specific mechanisms of injury deaths (e.g., drug poisoning) might be considered completely preventable and other mechanisms less preventable. In addition, the majority of risk factors do not occur randomly in populations; they are closely related to the social, demographic, environmental, economic, and geographic attributes of the neighborhoods in which persons live and work.§§§ However, from a health equity perspective, every state can be compared with the same benchmark rates regardless of demographic differences. If health disparities were eliminated, as is called for by Healthy People 2020,¶¶¶ all states could be closer to achieving the lowest possible death rates for the five leading causes of death. Further analysis of state and regional differences in death rates for the five leading causes of death could assist state and federal health officials in establishing prevention goals, priorities, and strategies. Clinical preventive services, including physician tobacco cessation counseling, as recommended by the U.S. Preventive Services Task Force**** for heart disease, stroke, cancer, and CLRD also provide opportunities for addressing preventable deaths.†††† AcknowledgmentsChad Heilig, PhD, Paul Z. Siegel, MD, Center for Surveillance, Epidemiology, and Laboratory Services, CDC; Peter Briss, MD, National Center for Chronic Disease Prevention and Health Promotion, CDC. Corresponding author: Macarena C. García, mcgarcia@cdc.gov, 404-539-4410. 1Center for Surveillance, Epidemiology, and Laboratory Services, CDC; 2National Center for Health Statistics, CDC; 3National Center for Injury Prevention and Control, CDC; 4National Center for Chronic Disease Prevention and Health Promotion, CDC. * http://www.cdc.gov/nchs/data/nvsr/nvsr61/nvsr61_04.pdf. † Diseases of the heart codes I00-I09, I11, I13, I20-I51; cancer C00-C97; CLRD J40-J47; cerebrovascular diseases (stroke) I60-I69; and unintentional injuries V01-X59, Y85-Y86. § Standard error = the square root of [expected number + observed number of deaths]. ¶ Region 1: Connecticut, Maine, Massachusetts, New Hampshire, Rhode Island, and Vermont. Region 2: New Jersey, New York, Puerto Rico, and the U.S. Virgin Islands. Region 3: Delaware, the District of Columbia, Maryland, Pennsylvania, Virginia, and West Virginia. Region 4: Alabama, Florida, Georgia, Kentucky, Mississippi, North Carolina, South Carolina, and Tennessee. Region 5: Illinois, Indiana, Michigan, Minnesota, Ohio, and Wisconsin. Region 6: Arkansas, Louisiana, New Mexico, Oklahoma, and Texas. Region 7: Iowa, Kansas, Missouri, and Nebraska. Region 8: Colorado, Montana, North Dakota, South Dakota, Utah, and Wyoming. Region 9: Arizona, California, Hawaii, Nevada, American Samoa, Commonwealth of the Northern Mariana Islands, Federated States of Micronesia, Guam, Marshall Islands, and Republic of Palau. Region 10: Alaska, Idaho, Oregon, and Washington. ** http://www.cdc.gov/nchs/data/databriefs/db220.pdf. ††http://www.surgeongeneral.gov/library/reports/50-years-of-progress/. §§http://www.cdc.gov/tobacco/stateandcommunity/best_practices/index.htm. ¶¶http://www.nhlbi.nih.gov/sites/www.nhlbi.nih.gov/files/obesity-evidence-review.pdf. *** http://www.cdc.gov/steadi/pdf/stay_independent_brochure-a.pdf. †††http://www.cdc.gov/nchs/products/vsrr/mortality-dashboard.htm. §§§http://www.cdc.gov/mmwr/preview/ind2013_su.html. ¶¶¶https://www.healthypeople.gov/. **** https://www.uspreventiveservicestaskforce.org/Page/Name/uspstf-a-and-b-recommendations/. References
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| HHS region | 2010 | 2014 | Z-test significance | ||||
|---|---|---|---|---|---|---|---|
| Expected | Observed | Potentially preventable | Expected | Observed | Potentially preventable | ||
| Diseases of the heart | |||||||
| 1 | 8,904 | 10,286 | 1,382 | 9,798 | 10,468 | 670 | * |
| 2 | 16,765 | 24,477 | 7,712 | 18,170 | 24,272 | 6,102 | * |
| 3 | 18,327 | 28,563 | 10,236 | 20,099 | 29,185 | 9,086 | * |
| 4 | 38,367 | 65,198 | 26,831 | 43,235 | 69,897 | 26,662 | |
| 5 | 30,726 | 47,280 | 16,554 | 33,618 | 50,437 | 16,819 | |
| 6 | 20,656 | 35,898 | 15,242 | 23,245 | 39,907 | 16,662 | * |
| 7 | 8,281 | 12,769 | 4,488 | 8,958 | 13,425 | 4,467 | |
| 8 | 5,782 | 6,464 | 682 | 6,616 | 7,325 | 709 | |
| 9 | 26,030 | 33,352 | 7,322 | 29,622 | 35,133 | 5,511 | * |
| 10 | 7,422 | 8,401 | 979 | 8,539 | 9,216 | 677 | |
| Malignant neoplasms (cancers) | |||||||
| 1 | 15,587 | 19,061 | 3,474 | 17,216 | 18,995 | 1,779 | * |
| 2 | 29,259 | 34,735 | 5,476 | 31,827 | 34,826 | 2,999 | * |
| 3 | 32,039 | 42,003 | 9,964 | 35,241 | 43,236 | 7,995 | * |
| 4 | 66,962 | 90,439 | 23,477 | 75,522 | 95,461 | 19,939 | * |
| 5 | 53,686 | 71,553 | 17,867 | 58,975 | 73,529 | 14,554 | * |
| 6 | 36,074 | 46,950 | 10,876 | 40,693 | 49,216 | 8,523 | * |
| 7 | 14,443 | 19,028 | 4,585 | 15,692 | 19,653 | 3,961 | |
| 8 | 10,123 | 10,708 | 585 | 11,625 | 11,387 | -238† | * |
| 9 | 45,439 | 50,611 | 5,172 | 51,835 | 53,179 | 1,344 | * |
| 10 | 13,041 | 15,861 | 2,820 | 15,018 | 16,700 | 1,682 | * |
| Cerebrovascular diseases (stroke) | |||||||
| 1 | 1,722 | 1,863 | 141 | 1,914 | 1,781 | -133 | * |
| 2 | 3,261 | 3,742 | 481 | 3,556 | 3,716 | 160 | * |
| 3 | 3,568 | 5,239 | 1,671 | 3,947 | 5,511 | 1,564 | |
| 4 | 7,538 | 12,960 | 5,422 | 8,567 | 13,934 | 5,367 | |
| 5 | 5,988 | 8,832 | 2,844 | 6,603 | 9,143 | 2,540 | |
| 6 | 4,040 | 7,174 | 3,134 | 4,575 | 7,749 | 3,174 | |
| 7 | 1,628 | 2,405 | 777 | 1,773 | 2,490 | 717 | |
| 8 | 1,128 | 1,374 | 246 | 1,302 | 1,440 | 138 | |
| 9 | 5,078 | 6,904 | 1,826 | 5,822 | 6,952 | 1,130 | * |
| 10 | 1,439 | 1,867 | 428 | 1,679 | 1,991 | 312 | |
| Chronic lower respiratory diseases (CLRD) | |||||||
| 1 | 2,234 | 2,774 | 540 | 2,505 | 3,068 | 563 | |
| 2 | 4,218 | 4,794 | 576 | 4,634 | 4,697 | 63 | * |
| 3 | 4,630 | 6,951 | 2,321 | 5,166 | 7,234 | 2,068 | |
| 4 | 9,820 | 18,612 | 8,792 | 11,254 | 21,025 | 9,771 | * |
| 5 | 7,740 | 13,494 | 5,754 | 8,623 | 14,669 | 6,046 | |
| 6 | 5,174 | 9,539 | 4,365 | 5,911 | 10,547 | 4,636 | |
| 7 | 2,111 | 4,318 | 2,207 | 2,317 | 4,644 | 2,327 | |
| 8 | 1,442 | 2,447 | 1,005 | 1,686 | 2,681 | 995 | |
| 9 | 6,514 | 8,447 | 1,933 | 7,550 | 8,977 | 1,427 | * |
| 10 | 1,857 | 3,082 | 1,225 | 2,195 | 3,357 | 1,162 | |
| Unintentional injuries (accidents) | |||||||
| 1 | 2,771 | 3,703 | 932 | 2,866 | 4,817 | 1,951 | * |
| 2 | 5,357 | 5,692 | 335 | 5,531 | 6,824 | 1,293 | * |
| 3 | 5,703 | 8,769 | 3,066 | 5,916 | 10,261 | 4,345 | * |
| 4 | 11,650 | 23,804 | 12,154 | 12,338 | 24,789 | 12,451 | |
| 5 | 9,724 | 15,104 | 5,380 | 9,984 | 17,898 | 7,914 | * |
| 6 | 7,040 | 13,487 | 6,447 | 7,530 | 14,598 | 7,068 | * |
| 7 | 2,566 | 4,720 | 2,154 | 2,639 | 4,901 | 2,262 | |
| 8 | 1,985 | 3,479 | 1,494 | 2,136 | 4,046 | 1,910 | * |
| 9 | 8,845 | 12,264 | 3,419 | 9,420 | 13,768 | 4,348 | * |
| 10 | 2,414 | 3,840 | 1,426 | 2,569 | 4,358 | 1,789 | * |
*Significant change from 2010 to 2014, p<0.01.
† Negative potentially preventable deaths occurred when an HHS region included one or more of the states with the lowest three death rates (the lowest three death rates were averaged to create the benchmark death rates) for at least a few age groups. Negative potentially preventable deaths are preserved in this table to test changes from 2010 to 2014.
 TABLE 2. Number of expected, observed, and potentially preventable deaths among the five leading causes of death and significant changes in potentially preventable deaths, for persons aged <80 years, by state — United States, 2010 and 2014
TABLE 2. Number of expected, observed, and potentially preventable deaths among the five leading causes of death and significant changes in potentially preventable deaths, for persons aged <80 years, by state — United States, 2010 and 2014
| State | 2010 | 2014 | Z-test significance | ||||
|---|---|---|---|---|---|---|---|
| Expected | Observed | Potentially preventable (95% CI) | Expected | Observed | Potentially preventable (95% CI) | ||
| Diseases of the heart | |||||||
| Alabama | 2,993 | 6,604 | 3,611 (3,419–3,803) | 3,266 | 6,933 | 3,667 (3,469–3,865) | |
| Alaska | 331 | 463 | 132 (77–187) | 377 | 497 | 120 (62–178) | |
| Arizona | 3,885 | 4,735 | 850 (668–1,032) | 4,512 | 5,061 | 549 (357–741) | |
| Arkansas | 1,845 | 3,808 | 1,963 (1,816–2,110) | 1,998 | 4,258 | 2,260 (2,105–2,415) | * |
| California | 19,742 | 24,707 | 4,965 (4,552–5,378) | 22,358 | 25,338 | 2,980 (2,552–3,408) | * |
| Colorado | 2,707 | 2,815 | 108 (-38–254) | 3,153 | 3,246 | 93 (-64–250) | |
| Connecticut | 2,176 | 2,569 | 393 (258–528) | 2,362 | 2,552 | 190 (53–327) | |
| Delaware | 575 | 857 | 282 (208–356) | 658 | 929 | 271 (193–349) | |
| District of Columbia | 310 | 729 | 419 (356–482) | 337 | 733 | 396 (332–460) | |
| Florida | 13,352 | 17,586 | 4,234 (3,889–4,579) | 15,121 | 19,121 | 4,000 (3,637–4,363) | |
| Georgia | 5,120 | 9,103 | 3,983 (3,749–4,217) | 5,890 | 9,911 | 4,021 (3,775–4,267) | |
| Hawaii | 836 | 1,007 | 171 (87–255) | 920 | 1,217 | 297 (206–388) | |
| Idaho | 883 | 1,080 | 197 (110–284) | 1,025 | 1,240 | 215 (122–308) | |
| Illinois | 7,249 | 11,424 | 4,175 (3,907–4,443) | 7,898 | 11,839 | 3,941 (3,666–4,216) | |
| Indiana | 3,783 | 6,421 | 2,638 (2,440–2,836) | 4,145 | 6,779 | 2,634 (2,429–2,839) | |
| Iowa | 1,892 | 2,716 | 824 (691–957) | 2,032 | 2,622 | 590 (456–724) | |
| Kansas | 1,636 | 2,248 | 612 (490–734) | 1,766 | 2,402 | 636 (509–763) | |
| Kentucky | 2,662 | 5,332 | 2,670 (2,495–2,845) | 2,912 | 5,798 | 2,886 (2,703–3,069) | |
| Louisiana | 2,609 | 5,784 | 3,175 (2,995–3,355) | 2,861 | 6,149 | 3,288 (3,102–3,474) | |
| Maine | 928 | 1,083 | 155 (67–243) | 1,026 | 1,167 | 141 (49–233) | |
| Maryland | 3,303 | 5,321 | 2,018 (1,836–2,200) | 3,701 | 5,476 | 1,775 (1,587–1,963) | |
| Massachusetts | 3,926 | 4,416 | 490 (311–669) | 4,333 | 4,382 | 49 (-134–232) | * |
| Michigan | 6,056 | 10,327 | 4,271 (4,020–4,522) | 6,646 | 11,461 | 4,815 (4,551–5,079) | * |
| Minnesota | 3,050 | 2,720 | -330† (-479 to -181) | 3,414 | 2,951 | -463 (-619 to -307) | |
| Mississippi | 1,750 | 4,183 | 2,433 (2,282–2,584) | 1,903 | 4,428 | 2,525 (2,369–2,681) | |
| Missouri | 3,691 | 6,553 | 2,862 (2,664–3,060) | 4,011 | 7,113 | 3,102 (2,895–3,309) | |
| Montana | 650 | 826 | 176 (101–251) | 733 | 910 | 177 (98–256) | |
| Nebraska | 1,063 | 1,252 | 189 (95–283) | 1,149 | 1,288 | 139 (42–236) | |
| Nevada | 1,566 | 2,903 | 1,337 (1,206–1,468) | 1,832 | 3,517 | 1,685 (1,542–1,828) | * |
| New Hampshire | 828 | 916 | 88 (6–170) | 931 | 976 | 45 (-41–131) | |
| New Jersey | 5,243 | 7,106 | 1,863 (1,645–2,081) | 5,703 | 7,145 | 1,442 (1,220–1,664) | * |
| New Mexico | 1,253 | 1,510 | 257 (154–360) | 1,382 | 1,642 | 260 (152–368) | |
| New York | 11,522 | 17,371 | 5,849 (5,516–6,182) | 12,467 | 17,127 | 4,660 (4,323–4,997) | * |
| North Carolina | 5,679 | 9,021 | 3,342 (3,104–3,580) | 6,456 | 9,223 | 2,767 (2,522–3,012) | * |
| North Dakota | 406 | 512 | 106 (47–165) | 437 | 542 | 105 (44–166) | |
| Ohio | 7,164 | 11,875 | 4,711 (4,441–4,981) | 7,736 | 12,697 | 4,961 (4,681–5,241) | |
| Oklahoma | 2,267 | 4,857 | 2,590 (2,425–2,755) | 2,456 | 5,300 | 2,844 (2,671–3,017) | |
| Oregon | 2,364 | 2,421 | 58 (-79–193) | 2,714 | 2,622 | -92 (-235–51) | |
| Pennsylvania | 8,221 | 12,668 | 4,447 (4,164–4,730) | 8,824 | 12,689 | 3,865 (3,578–4,152) | * |
| Rhode Island | 636 | 820 | 184 (109–259) | 689 | 855 | 166 (89–243) | |
| South Carolina | 2,896 | 5,413 | 2,517 (2,338–2,696) | 3,335 | 5,742 | 2,407 (2,220–2,594) | |
| South Dakota | 491 | 590 | 99 (35–163) | 541 | 741 | 200 (130–270) | |
| Tennessee | 3,916 | 7,956 | 4,040 (3,826–4,254) | 4,353 | 8,741 | 4,388 (4,164–4,612) | |
| Texas | 12,683 | 19,939 | 7,256 (6,902–7,610) | 14,549 | 22,558 | 8,009 (7,631–8,387) | * |
| Utah | 1,194 | 1,229 | 35 (-61–131) | 1,383 | 1,349 | -34 (-136–68) | |
| Vermont | 411 | 482 | 71 (12–130) | 457 | 536 | 79 (17–141) | |
| Virginia | 4,609 | 6,588 | 1,979 (1,772–2,186) | 5,185 | 6,978 | 1,793 (1,577–2,009) | |
| Washington | 3,844 | 4,437 | 593 (415–771) | 4,424 | 4,857 | 433 (244–622) | |
| West Virginia | 1,308 | 2,400 | 1,092 (973–1,211) | 1,395 | 2,380 | 985 (865–1,105) | |
| Wisconsin | 3,424 | 4,513 | 1,089 (914–1,264) | 3,779 | 4,710 | 931 (750–1,112) | |
| Wyoming | 333 | 492 | 159 (103–215) | 369 | 537 | 168 (109–227) | |
| United States | 181,261 | 272,688 | 91,757 (90,436–93,078) | 201,902 | 289,265 | 87,950 (86,576–89,324) | * |
| Malignant neoplasms (cancers) | |||||||
| Alabama | 5,227 | 7,595 | 2,368 (2,146–2,590) | 5,714 | 7,796 | 2,082 (1,854–2,310) | |
| Alaska | 588 | 703 | 115 (45–185) | 670 | 782 | 112 (37–187) | |
| Arizona | 6,775 | 7,460 | 685 (451–919) | 7,857 | 8,085 | 228 (-19–475) | * |
| Arkansas | 3,219 | 4,720 | 1,501 (1,326–1,676) | 3,487 | 4,897 | 1,410 (1,231–1,589) | |
| California | 34,454 | 38,226 | 3,772 (3,244–4,300) | 39,157 | 39,678 | 521 (-29–1071) | * |
| Colorado | 4,752 | 4,944 | 192 (-1–385) | 5,553 | 5,188 | -365 (-568 to -162) | * |
| Connecticut | 3,805 | 4,367 | 562 (385–739) | 4,144 | 4,219 | 75 (-104–254) | * |
| Delaware | 1,006 | 1,352 | 346 (251–441) | 1,151 | 1,426 | 275 (176–374) | |
| District of Columbia | 543 | 742 | 199 (129–269) | 592 | 837 | 245 (171–319) | |
| Florida | 23,195 | 28,249 | 5,054 (4,609–5,499) | 26,279 | 29,519 | 3,240 (2,777–3,703) | * |
| Georgia | 8,967 | 11,820 | 2,853 (2,570–3,136) | 10,323 | 12,738 | 2,415 (2,117–2,713) | |
| Hawaii | 1,467 | 1,555 | 88 (-20–196) | 1,616 | 1,693 | 77 (-36–190) | |
| Idaho | 1,546 | 1,753 | 207 (94–320) | 1,796 | 1,995 | 199 (78–320) | |
| Illinois | 12,654 | 16,558 | 3,904 (3,569–4,239) | 13,840 | 16,862 | 3,022 (2,679–3,365) | * |
| Indiana | 6,612 | 9,385 | 2,773 (2,525–3,021) | 7,268 | 9,821 | 2,553 (2,297–2,809) | |
| Iowa | 3,295 | 4,127 | 832 (663–1,001) | 3,559 | 4,258 | 699 (526–872) | |
| Kansas | 2,854 | 3,624 | 770 (612–928) | 3,098 | 3,758 | 660 (498–822) | |
| Kentucky | 4,655 | 7,499 | 2,844 (2,628–3,060) | 5,104 | 7,815 | 2,711 (2,488–2,934) | |
| Louisiana | 4,562 | 6,909 | 2,347 (2,137–2,557) | 5,021 | 7,137 | 2,116 (1,900–2,332) | |
| Maine | 1,627 | 2,259 | 632 (510–754) | 1,805 | 2,186 | 381 (257–505) | * |
| Maryland | 5,788 | 7,218 | 1,430 (1,206–1,654) | 6,499 | 7,616 | 1,117 (884–1,350) | |
| Massachusetts | 6,865 | 8,319 | 1,454 (1,212–1,696) | 7,609 | 8,341 | 732 (484–980) | * |
| Michigan | 10,600 | 14,394 | 3,794 (3,484–4,104) | 11,671 | 14,884 | 3,213 (2,894–3,532) | |
| Minnesota | 5,328 | 6,273 | 945 (734–1,156) | 5,992 | 6,267 | 275 (58–492) | * |
| Mississippi | 3,055 | 4,731 | 1,676 (1,503–1,849) | 3,330 | 5,019 | 1,689 (1,510–1,868) | |
| Missouri | 6,442 | 9,023 | 2,581 (2,337–2,825) | 7,020 | 9,345 | 2,325 (2,074–2,576) | |
| Montana | 1,143 | 1,304 | 161 (64–258) | 1,291 | 1,445 | 154 (51–257) | |
| Nebraska | 1,852 | 2,254 | 402 (276–528) | 2,014 | 2,292 | 278 (149–407) | |
| Nevada | 2,743 | 3,370 | 627 (474–780) | 3,205 | 3,723 | 518 (355–681) | |
| New Hampshire | 1,455 | 1,772 | 317 (206–428) | 1,642 | 1,846 | 204 (88–320) | |
| New Jersey | 9,147 | 10,948 | 1,801 (1,523–2,079) | 9,986 | 10,965 | 979 (695–1,263) | * |
| New Mexico | 2,194 | 2,393 | 199 (66–332) | 2,423 | 2,451 | 28 (-109–165) | |
| New York | 20,112 | 23,787 | 3,675 (3,264–4,086) | 21,842 | 23,861 | 2,019 (1,600–2,438) | * |
| North Carolina | 9,931 | 13,297 | 3,366 (3,067–3,665) | 11,304 | 14,393 | 3,089 (2,775–3,403) | |
| North Dakota | 708 | 780 | 72 (-4–148) | 767 | 852 | 85 (6–164) | |
| Ohio | 12,514 | 17,413 | 4,899 (4,560–5,238) | 13,570 | 18,043 | 4,473 (4,125–4,821) | |
| Oklahoma | 3,957 | 5,787 | 1,830 (1,637–2,023) | 4,293 | 5,896 | 1,603 (1,405–1,801) | |
| Oregon | 4,153 | 5,212 | 1,059 (869–1,249) | 4,771 | 5,496 | 725 (526–924) | |
| Pennsylvania | 14,340 | 19,114 | 4,774 (4416–5,132) | 15,463 | 19,064 | 3,601 (3,237–3,965) | * |
| Rhode Island | 1,112 | 1,423 | 311 (212–410) | 1,210 | 1,442 | 232 (131–333) | |
| South Carolina | 5,079 | 7,063 | 1,984 (1,768–2,200) | 5,846 | 7,487 | 1,641 (1,415–1,867) | |
| South Dakota | 856 | 1,054 | 198 (112–284) | 950 | 1,115 | 165 (76–254) | |
| Tennessee | 6,853 | 10,185 | 3,332 (3,076–3,588) | 7,622 | 10,694 | 3,072 (2,807–3,337) | |
| Texas | 22,143 | 27,141 | 4,998 (4,563–5,433) | 25,469 | 28,835 | 3,366 (2,909–3,823) | * |
| Utah | 2,080 | 1,931 | -149 (-273 to -25) | 2,413 | 2,105 | -308 (-440 to -176) | |
| Vermont | 723 | 921 | 198 (119–277) | 807 | 961 | 154 (72–236) | |
| Virginia | 8,073 | 1,0162 | 2,089 (1,824–2,354) | 9090 | 10,651 | 1,561 (1,286–1,836) | * |
| Washington | 6,754 | 8,193 | 1,439 (1,199–1,679) | 7,781 | 8,427 | 646 (396–896) | * |
| West Virginia | 2,289 | 3,415 | 1,126 (978–1,274) | 2,446 | 3,642 | 1,196 (1,043–1,349) | |
| Wisconsin | 5,978 | 7,530 | 1,552 (1,324–1,780) | 6,635 | 7,652 | 1,017 (783–1251) | * |
| Wyoming | 585 | 695 | 110 (40–180) | 651 | 682 | 31 (-41–103) | |
| United States | 316,652 | 400,949 | 84,443 (82,783–86,103) | 353,645 | 416,182 | 63,209 (61,489–64,929) | * |
| Cerebrovascular diseases (stroke) | |||||||
| Alabama | 588 | 1,277 | 689 (604–774) | 646 | 1,335 | 689 (602–776) | |
| Alaska | 62 | 91 | 29 (5–53) | 72 | 87 | 15 (-10–40) | |
| Arizona | 771 | 848 | 77 (-2–156) | 905 | 912 | 7 (-77–91) | |
| Arkansas | 365 | 718 | 353 (289–417) | 398 | 738 | 340 (274–406) | |
| California | 3,839 | 5,366 | 1,527 (1,339–1,715) | 4,374 | 5,324 | 950 (757–1,143) | * |
| Colorado | 520 | 604 | 84 (18–150) | 614 | 633 | 19 (-50–88) | |
| Connecticut | 420 | 425 | 5 (-52–62) | 460 | 405 | -55 (-113–3) | |
| Delaware | 113 | 170 | 57 (24–90) | 130 | 172 | 42 (8–76) | |
| District of Columbia | 61 | 107 | 46 (21–71) | 66 | 88 | 22 (-2–46) | |
| Florida | 2,655 | 3,481 | 826 (672–980) | 3,030 | 3,812 | 782 (620–944) | |
| Georgia | 989 | 1,965 | 976 (869–1,083) | 1,150 | 2,060 | 910 (799–1,021) | |
| Hawaii | 163 | 244 | 81 (41–121) | 182 | 234 | 52 (12–92) | |
| Idaho | 174 | 234 | 60 (20–100) | 204 | 268 | 64 (21–107) | |
| Illinois | 1,412 | 2,047 | 635 (520–750) | 1,547 | 2,175 | 628 (508–748) | |
| Indiana | 739 | 1,240 | 501 (414–588) | 816 | 1,289 | 473 (383–563) | |
| Iowa | 373 | 462 | 89 (32–146) | 403 | 465 | 62 (4–120) | |
| Kansas | 321 | 485 | 164 (108–220) | 349 | 489 | 140 (83–197) | |
| Kentucky | 520 | 934 | 414 (339–489) | 573 | 948 | 375 (299–451) | |
| Louisiana | 510 | 1,003 | 493 (417–569) | 564 | 1,176 | 612 (530–694) | |
| Maine | 180 | 229 | 49 (9–89) | 202 | 222 | 20 (-20–60) | |
| Maryland | 636 | 935 | 299 (221–377) | 720 | 1,025 | 305 (223–387) | |
| Massachusetts | 761 | 807 | 46 (-32–124) | 846 | 784 | -62 (-141–17) | |
| Michigan | 1,178 | 1,743 | 565 (459–671) | 1,306 | 1,792 | 486 (377–595) | |
| Minnesota | 592 | 662 | 70 (1–139) | 669 | 705 | 36 (-37–109) | |
| Mississippi | 344 | 827 | 483 (416–550) | 377 | 858 | 481 (412–550) | |
| Missouri | 724 | 1,164 | 440 (355–525) | 793 | 1,263 | 470 (381–559) | |
| Montana | 127 | 162 | 35 (2–68) | 146 | 182 | 36 (1–71) | |
| Nebraska | 209 | 294 | 85 (41–129) | 227 | 273 | 46 (2–90) | |
| Nevada | 305 | 446 | 141 (87–195) | 361 | 482 | 121 (64–178) | |
| New Hampshire | 158 | 163 | 5 (-30–40) | 181 | 174 | -7 (-44–30) | |
| New Jersey | 1,015 | 1,319 | 304 (209–399) | 1,111 | 1,322 | 211 (114–308) | |
| New Mexico | 246 | 310 | 64 (18–110) | 275 | 321 | 46 (-2–94) | |
| New York | 2,246 | 2,423 | 177 (43–311) | 2,445 | 2,394 | -51 (-187–85) | |
| North Carolina | 1,108 | 1,894 | 786 (679–893) | 1,271 | 2,110 | 839 (725–953) | |
| North Dakota | 80 | 127 | 47 (19–75) | 87 | 120 | 33 (5–61) | |
| Ohio | 1,400 | 2,271 | 871 (752–990) | 1,523 | 2,328 | 805 (683–927) | |
| Oklahoma | 448 | 889 | 441 (369–513) | 488 | 894 | 406 (333–479) | |
| Oregon | 461 | 635 | 174 (109–239) | 536 | 699 | 163 (94–232) | |
| Pennsylvania | 1,611 | 2,194 | 583 (462–704) | 1,740 | 2,388 | 648 (522–774) | |
| Rhode Island | 123 | 148 | 25 (-7–57) | 135 | 114 | -21 (-52–10) | |
| South Carolina | 567 | 1,119 | 552 (472–632) | 661 | 1,185 | 524 (440–608) | |
| South Dakota | 97 | 126 | 29 (0–58) | 107 | 108 | 1 (-28–30) | |
| Tennessee | 765 | 1,463 | 698 (605–791) | 859 | 1,626 | 767 (669–865) | |
| Texas | 2,471 | 4,254 | 1,783 (1,622–1,944) | 2,850 | 4,620 | 1,770 (1,601–1,939) | |
| Utah | 238 | 282 | 44 (-1–89) | 276 | 325 | 49 (1–97) | |
| Vermont | 79 | 91 | 12 (-14–38) | 90 | 82 | -8 (-34–18) | |
| Virginia | 891 | 1,369 | 478 (385–571) | 1,014 | 1,354 | 340 (245–435) | |
| Washington | 743 | 907 | 164 (84–244) | 867 | 937 | 70 (-13–153) | |
| West Virginia | 257 | 464 | 207 (154–260) | 276 | 484 | 208 (154–262) | |
| Wisconsin | 667 | 869 | 202 (125–279) | 742 | 854 | 112 (34–190) | |
| Wyoming | 65 | 73 | 8 (-15–31) | 73 | 72 | -1 (-25–23) | |
| United States | 35,390 | 52,360 | 16,973 (16,392–17,554) | 39,737 | 54,707 | 15,175 (14,573–15,777) | * |
| Chronic lower respiratory diseases (CLRD) | |||||||
| Alabama | 765 | 1,778 | 1,013 (914–1,112) | 848 | 1,897 | 1,049 (946–1,152) | |
| Alaska | 77 | 112 | 35 (8–62) | 92 | 116 | 24 (-4–52) | |
| Arizona | 1,004 | 1,558 | 554 (455–653) | 1,189 | 1,870 | 681 (573–789) | |
| Arkansas | 476 | 1,101 | 625 (547–703) | 523 | 1,339 | 816 (731–901) | * |
| California | 4,904 | 6,047 | 1,143 (938–1,348) | 5,650 | 6,073 | 423 (211–635) | * |
| Colorado | 665 | 1,141 | 476 (393–559) | 795 | 1,301 | 506 (416–596) | |
| Connecticut | 544 | 509 | -35 (-99–29) | 601 | 586 | -15 (-83–53) | |
| Delaware | 147 | 224 | 77 (39–115) | 172 | 231 | 59 (20–98) | |
| District of Columbia | 78 | 73 | -5 (-29–19) | 85 | 73 | -12 (-37–13) | |
| Florida | 3,501 | 5,327 | 1,826 (1,642–2,010) | 4,018 | 5,855 | 1,837 (1,642–2,032) | |
| Georgia | 1,263 | 2,413 | 1,150 (1,031–1,269) | 1,486 | 2,729 | 1,243 (1,116–1,370) | |
| Hawaii | 212 | 141 | -71 (-108 to -34) | 239 | 151 | -88 (-127 to -49) | |
| Idaho | 224 | 409 | 185 (136–234) | 267 | 485 | 218 (164–272) | |
| Illinois | 1,815 | 2,740 | 925 (793–1,057) | 2,010 | 2,891 | 881 (744–1,018) | |
| Indiana | 954 | 2,154 | 1,200 (1,091–1,309) | 1,063 | 2,389 | 1,326 (1,211–1,441) | |
| Iowa | 485 | 859 | 374 (302–446) | 528 | 968 | 440 (364–516) | |
| Kansas | 414 | 826 | 412 (343–481) | 455 | 938 | 483 (410–556) | |
| Kentucky | 675 | 1,792 | 1,117 (1,020–1,214) | 750 | 2,078 | 1,328 (1,224–1,432) | * |
| Louisiana | 658 | 1,106 | 448 (366–530) | 733 | 1,360 | 627 (537–717) | * |
| Maine | 237 | 443 | 206 (155–257) | 268 | 494 | 226 (172–280) | |
| Maryland | 818 | 1,035 | 217 (133–301) | 936 | 998 | 62 (-24–148) | |
| Massachusetts | 984 | 1,115 | 131 (41–221) | 1,105 | 1,205 | 100 (6–194) | |
| Michigan | 1,527 | 2,721 | 1,194 (1,066–1,322) | 1,712 | 2,939 | 1,227 (1,093–1,361) | |
| Minnesota | 762 | 960 | 198 (117–279) | 871 | 1,153 | 282 (194–370) | |
| Mississippi | 446 | 1,016 | 570 (495–645) | 492 | 1,129 | 637 (558–716) | |
| Missouri | 941 | 2,090 | 1,149 (1,041–1,257) | 1,039 | 2,175 | 1,136 (1025–1,247) | |
| Montana | 166 | 341 | 175 (131–219) | 192 | 380 | 188 (141–235) | |
| Nebraska | 270 | 543 | 273 (217–329) | 296 | 563 | 267 (210–324) | |
| Nevada | 395 | 701 | 306 (241–371) | 472 | 883 | 411 (339–483) | |
| New Hampshire | 206 | 315 | 109 (64–154) | 237 | 352 | 115 (67–163) | |
| New Jersey | 1,312 | 1,436 | 124 (21–227) | 1,447 | 1,391 | -56 (-160–48) | |
| New Mexico | 320 | 535 | 215 (158–272) | 361 | 605 | 244 (183–305) | |
| New York | 2,906 | 3,358 | 452 (297–607) | 3,186 | 3,306 | 120 (-38–278) | * |
| North Carolina | 1,436 | 2,698 | 1,262 (1,136–1,388) | 1,663 | 3,077 | 1,414 (1,279–1,549) | |
| North Dakota | 104 | 170 | 66 (34–98) | 113 | 162 | 49 (17–81) | |
| Ohio | 1,818 | 3,729 | 1,911 (1,765–2,057) | 1,996 | 3,922 | 1,926 (1,775–2,077) | |
| Oklahoma | 581 | 1,736 | 1,155 (1,061–1,249) | 638 | 1,787 | 1,149 (1,052–1,246) | |
| Oregon | 599 | 1,110 | 511 (430–592) | 706 | 1,153 | 447 (363–531) | |
| Pennsylvania | 2,101 | 3,051 | 950 (809–1,091) | 2,287 | 3,223 | 936 (791–1,081) | |
| Rhode Island | 160 | 225 | 65 (27–103) | 176 | 242 | 66 (26–106) | |
| South Carolina | 740 | 1,391 | 651 (561–741) | 870 | 1,693 | 823 (724–922) | |
| South Dakota | 126 | 226 | 100 (63–137) | 140 | 202 | 62 (26–98) | |
| Tennessee | 995 | 2,197 | 1,202 (1,091–1,313) | 1,125 | 2,567 | 1,442 (1,323–1,561) | * |
| Texas | 3,139 | 5,061 | 1,922 (1,745–2,099) | 3,656 | 5,456 | 1,800 (1,613–1,987) | |
| Utah | 298 | 383 | 85 (34–136) | 350 | 451 | 101 (46–156) | |
| Vermont | 103 | 167 | 64 (32–96) | 118 | 189 | 71 (37–105) | |
| Virginia | 1,148 | 1,647 | 499 (395–603) | 1,320 | 1,714 | 394 (286–502) | |
| Washington | 956 | 1,451 | 495 (399–591) | 1,130 | 1,603 | 473 (371–575) | |
| West Virginia | 338 | 921 | 583 (513–653) | 367 | 995 | 628 (556–700) | |
| Wisconsin | 862 | 1,190 | 328 (239–417) | 970 | 1,375 | 405 (310–500) | |
| Wyoming | 83 | 186 | 103 (71–135) | 95 | 185 | 90 (57–123) | |
| United States | 45,738 | 74,458 | 28,831 (28,151–29,511) | 51,840 | 80,899 | 29,232 (28,518–29,946) | |
| Unintentional injuries (accidents) | |||||||
| Alabama | 910 | 2,036 | 1,126 (1,020–1,232) | 939 | 2,104 | 1,165 (1,057–1,273) | |
| Alaska | 131 | 331 | 200 (158–242) | 137 | 348 | 211 (168–254) | |
| Arizona | 1,191 | 2,341 | 1,150 (1,034–1,266) | 1,284 | 2,562 | 1,278 (1,156–1,400) | |
| Arkansas | 551 | 1,221 | 670 (587–753) | 568 | 1,172 | 604 (522–686) | |
| California | 6,886 | 8,627 | 1,741 (1,497–1,985) | 7,315 | 9,818 | 2,503 (2,246–2,760) | * |
| Colorado | 940 | 1,525 | 585 (488–682) | 1,018 | 1,833 | 815 (710–920) | * |
| Connecticut | 679 | 905 | 226 (148–304) | 696 | 1,142 | 446 (362–530) | * |
| Delaware | 172 | 296 | 124 (82–166) | 183 | 350 | 167 (122–212) | |
| District of Columbia | 117 | 169 | 52 (19–85) | 128 | 177 | 49 (15–83) | |
| Florida | 3,675 | 6,927 | 3,252 (3,050–3,454) | 3,951 | 6,997 | 3,046 (2,841–3,251) | |
| Georgia | 1,791 | 3,133 | 1,342 (1,204–1,480) | 1,905 | 3,342 | 1,437 (1,295–1,579) | |
| Hawaii | 259 | 344 | 85 (37–133) | 272 | 356 | 84 (35–133) | |
| Idaho | 285 | 516 | 231 (176–286) | 304 | 575 | 271 (213–329) | |
| Illinois | 2,395 | 3,093 | 698 (553–843) | 2,449 | 3,642 | 1,193 (1,040–1,346) | * |
| Indiana | 1,209 | 2,064 | 855 (743–967) | 1,250 | 2,425 | 1,175 (1,056–1,294) | * |
| Iowa | 571 | 892 | 321 (246–396) | 587 | 948 | 361 (284–438) | |
| Kansas | 525 | 1,010 | 485 (408–562) | 539 | 1,004 | 465 (388–542) | |
| Kentucky | 826 | 2,240 | 1,414 (1,305–1,523) | 852 | 2,225 | 1,373 (1,264–1,482) | |
| Louisiana | 850 | 1,771 | 921 (821–1,021) | 882 | 2,074 | 1,192 (1,085–1,299) | * |
| Maine | 262 | 390 | 128 (78–178) | 267 | 487 | 220 (166–274) | |
| Maryland | 1,093 | 1,065 | -28 (-119–63) | 1,147 | 1,217 | 70 (-25–165) | |
| Massachusetts | 1,252 | 1,507 | 255 (152–358) | 1,310 | 2,085 | 775 (661–889) | * |
| Michigan | 1,869 | 2,923 | 1,054 (918–1,190) | 1,916 | 3,455 | 1,539 (1,395–1,683) | * |
| Minnesota | 993 | 1,342 | 349 (254–444) | 1,034 | 1,440 | 406 (309–503) | |
| Mississippi | 553 | 1,395 | 842 (756–928) | 567 | 1,438 | 871 (783–959) | |
| Missouri | 1,133 | 2,328 | 1,195 (1,080–1,310) | 1,164 | 2,414 | 1,250 (1,133–1,367) | |
| Montana | 190 | 416 | 226 (178–274) | 199 | 418 | 219 (170–268) | |
| Nebraska | 337 | 490 | 153 (97–209) | 349 | 535 | 186 (128–244) | |
| Nevada | 510 | 952 | 442 (367–517) | 549 | 1,032 | 483 (405–561) | |
| New Hampshire | 255 | 381 | 126 (77–175) | 263 | 507 | 244 (190–298) | * |
| New Jersey | 1,665 | 1,888 | 223 (106–340) | 1,718 | 2,309 | 591 (467–715) | * |
| New Mexico | 386 | 1,013 | 627 (554–700) | 397 | 1,249 | 852 (772–932) | * |
| New York | 3,692 | 3,804 | 112 (-58–282) | 3,813 | 4,515 | 702 (523–881) | * |
| North Carolina | 1,802 | 3,268 | 1,466 (1,326–1,606) | 1,915 | 3,592 | 1,677 (1,532–1,822) | |
| North Dakota | 127 | 193 | 66 (31–101) | 138 | 233 | 95 (57–133) | |
| Ohio | 2,184 | 4,016 | 1,832 (1,678–1,986) | 2,230 | 4,928 | 2,698 (2,532–2,864) | * |
| Oklahoma | 703 | 1,870 | 1,167 (1,068–1,266) | 732 | 1,944 | 1,212 (1,111–1,313) | |
| Oregon | 730 | 1,068 | 338 (255–421) | 773 | 1,254 | 481 (393–569) | |
| Pennsylvania | 2,435 | 4,319 | 1,884 (1,723–2,045) | 2,486 | 4,993 | 2,507 (2,337–2,677) | * |
| Rhode Island | 200 | 339 | 139 (93–185) | 205 | 408 | 203 (154–252) | |
| South Carolina | 883 | 1,910 | 1,027 (923–1,131) | 942 | 2,032 | 1,090 (983–1,197) | |
| South Dakota | 151 | 284 | 133 (92–174) | 159 | 320 | 161 (118–204) | |
| Tennessee | 1,209 | 2,895 | 1,686 (1,560–1,812) | 1,268 | 3,059 | 1,791 (1,662–1,920) | |
| Texas | 4,551 | 7,612 | 3,061 (2,845–3,277) | 4,951 | 8,159 | 3,208 (2,984–3,432) | |
| Utah | 470 | 765 | 295 (226–364) | 510 | 927 | 417 (343–491) | |
| Vermont | 122 | 181 | 59 (25–93) | 125 | 188 | 63 (28–98) | |
| Virginia | 1,521 | 1,889 | 368 (254–482) | 1,604 | 2,390 | 786 (662–910) | * |
| Washington | 1,269 | 1,925 | 656 (545–767) | 1,355 | 2,181 | 826 (709–943) | |
| West Virginia | 364 | 1,031 | 667 (594–740) | 368 | 1,134 | 766 (690–842) | |
| Wisconsin | 1,074 | 1,666 | 592 (489–695) | 1,105 | 2,008 | 903 (794–1,012) | * |
| Wyoming | 106 | 296 | 190 (151–229) | 111 | 315 | 204 (164–244) | |
| United States | 58,055 | 94,862 | 36,836 (36,070–37,602) | 60,929 | 106,260 | 45,331 (44,530–46,132) | * |
Abbreviation: CI = confidence interval.
*Significant change from 2010 to 2014, p<0.01.
† Negative potentially preventable deaths occurred when a U.S. Department of Health and Human Services region included one or more of the states with the lowest three death rates (the lowest three death rates were averaged to create the benchmark death rates) for at least a few age groups. Negative potentially preventable deaths were preserved in this table to test changes from 2010 to 2014, but were truncated to zero and not included in the totals for the United States in the table and text.
Suggested citation for this article: García MC, Bastian B, Rossen LM, et al. Potentially Preventable Deaths Among the Five Leading Causes of Death — United States, 2010 and 2014. MMWR Morb Mortal Wkly Rep 2016;65:1245–1255. DOI: http://dx.doi.org/10.15585/mmwr.mm6545a1.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of Health and Human Services.
References to non-CDC sites on the Internet are provided as a service to MMWR readers and do not constitute or imply endorsement of these organizations or their programs by CDC or the U.S. Department of Health and Human Services. CDC is not responsible for the content of pages found at these sites. URL addresses listed in MMWR were current as of the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.
Source URL: https://www.cdc.gov/mmwr/volumes/65/wr/mm6545a1.htm
Source Agency: Centers for Disease Control and Prevention (CDC)
Captured Date: 2016-11-18 01:46:56.0